Copyright © 2022 Foshan MBRT Nanofiberlabs Technology Co., Ltd All rights reserved.Site Map
Recently, the groups of Mi Shengli and Sun Wei, users of Tsinghua University Shenzhen International Graduate School of Foshan Lepton Precision Measurement and Control Technology Co., Ltd. have made significant progress in the field of corneal stroma induction regeneration. The related results were published in Nature Communications on March 18, 2020. "(Nature Communications), titled "Fiber reinforced GelMA hydrogel to induce the regeneration of corneal stroma".

As a vital tissue in the visual imaging system, the cornea is the convex and highly transparent substance at the front of the eye, which can protect the microstructure and tissues in the eye and provide most of the refractive power for the eye. However, corneal injury, infection and some congenital factors have caused corneal disease to become the second most common blind disease in the world. Allogeneic cornea, artificial cornea and human amniotic membrane transplantation are the three most widely used clinical treatment methods for corneal diseases, but these methods have certain problems or defects. Therefore, it is very important to use advanced biofabrication to develop a therapeutic corneal stent that can replace the corneal tissue affected by the disease or induce the corneal tissue to regenerate itself. At present, the difficulty in inducing regeneration of corneal tissue lies in the corneal stromal layer, which is the main component of the cornea. It has a complex structure composed of multiple orthogonally oriented nanofiber laminae, which is difficult to simulate truthfully using traditional bioengineering methods. The structure of the matrix layer. There are corneal stromal cells distributed between the fibrous lamellae, which are easily transformed into corneal fibroblasts and myofibroblasts when cultured in vitro and corneal tissue is damaged, leading to scarring of the cornea. Therefore, preparing a scaffold that can mimic the structure of the natural corneal stroma while maintaining the phenotype of corneal stroma cells and inducing the regeneration of the corneal stroma is a major challenge.
In response to this problem, Mi Shengli and Sun Wei’s research group proposed the use of near-field electrospinning technology to prepare grid-like sub-micron fiber scaffolds, and combined with hydrogel technology to prepare fiber-hydrogel composite scaffolds. Simulates the orthogonally oriented corneal stroma lamellar structure and glycoprotein that connects the lamellar layers. The research group proposed an optimal combination of topological structure and chemical factors, which can inhibit the fibroblast differentiation of corneal stromal cells, maintain their phenotype, and finally achieve the induced regeneration of the corneal stroma.
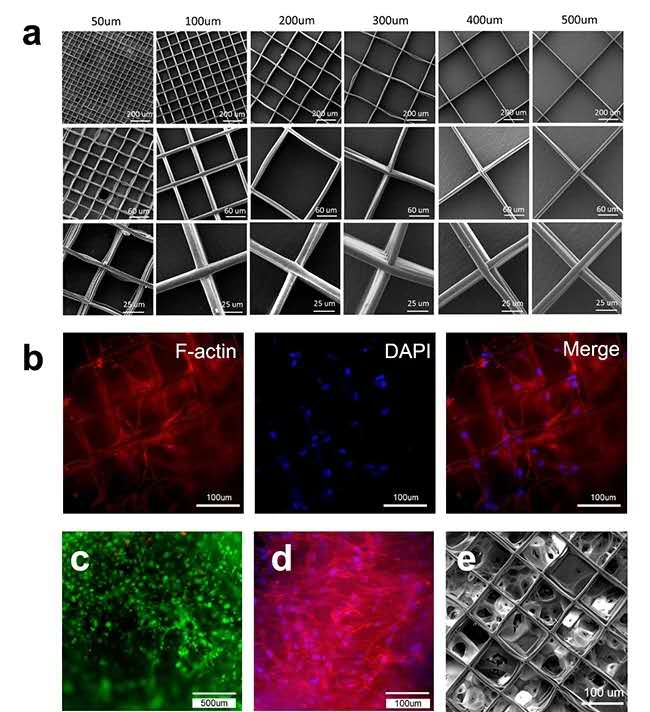
Figure 1: (a) SEM pictures of PECL grid-like submicron fiber scaffolds with different fiber spacings prepared by near-field electrospinning technology under different magnifications; (b) cornea seeded on 100um grid-like fiber scaffolds Limbal stromal stem cells are stained for cytoskeleton and nucleus, and the cells can grow along the fiber direction on the scaffold; (c) Limbal stromal stem cells encapsulated in 5% GelMA hydrogel are stained alive and dead; (d) 5% GelMA water The cytoskeleton and nucleus staining image of limbal stem cells encapsulated in the gel; (e) SEM image of the fiber-hydrogel composite scaffold.
At present, the most widely used material for near-field electrospinning technology is PCL, but because PCL is a hydrophobic material, it is not conducive to cell adhesion. Therefore, this study used PEG as an initiator to synthesize PECL, a copolymer of PEG and PCL, which significantly improved The hydrophilicity of PCL. For the first time, the research group successfully prepared an orthogonally oriented PECL submicron fiber scaffold using near-field electrospinning technology (Figure 1a). Limbal stromal stem cells can adhere to the surface of the scaffold and spread and grow along the fiber direction (Figure 1b).
The study synthesized GelMA by modifying MA to the gelatin macromolecular chain, and explored the optimal MA modification degree and GelMA concentration, which can make the limbal stromal stem cells encapsulated in GelMA hydrogel maintain high cell viability (Figure 1c) And can be spread out (Figure 1d).
The research group prepared the fiber-hydrogel composite scaffold by mold infusion (Figure 1e). By studying the effect of grid-like scaffolds with different fiber spacing on the physical and chemical properties of the fiber-hydrogel composite scaffold, the optimal topology was found. It can make the fiber hydrogel closest to the natural corneal tissue in terms of mechanical properties, light transmittance and swelling. Study the inoculation of limbal stromal stem cells in 2D cell culture dishes, 3D GelMA hydrogel and optimal fiber hydrogel composite scaffold, and study the effects of limbal stromal stem cells in serum-containing and serum-free medium Differentiation and maintenance of corneal stromal cell phenotype. Studies have shown that this optimal fiber hydrogel topology and serum-free medium can inhibit the differentiation of corneal stromal cells into fibroblasts.
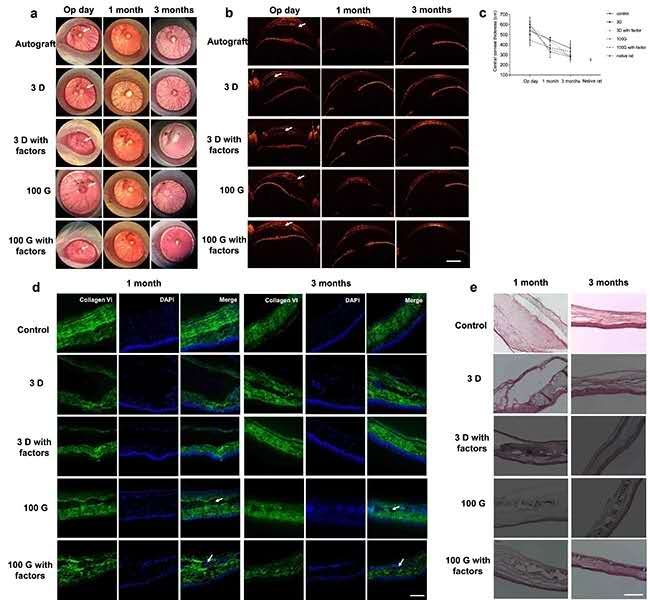
Figure 2 Rat corneal intrastromal lamellar transplantation experiment and evaluation: (a) Slit lamp observation picture after 5 kinds of stent transplantation; (b) OCT observation picture after stent transplantation, the scale is 1000um; (c) The center of different time periods after stent transplantation Corneal thickness; (d) 1 month and 3 months postoperative immunofluorescence staining pictures to observe the tissue induced regeneration, the scale is 100um; (e) 1 month and 3 months postoperative HE staining pictures to observe the tissue induced regeneration , The scale is 100um.
Finally, the study uses rats to carry out lamellar transplantation experiments in the cornea. The transplantation of 3D GelMA hydrogel, 3D GelMA containing chemical factors, optimal fibrous hydrogel scaffold and optimal fibrous hydrogel scaffold containing chemical factors were carried out respectively. , The control group was autologous corneal transplantation (Figure 2a). After 3 months of research and observation by OCT, immunofluorescence staining and HE staining after surgery (Figure 2b-e), it was found that compared with other stents, the transplantation of the optimal fiber hydrogel stent containing chemical factors can be best achieved Induced regeneration of corneal stroma.
The first authors of the paper are Tsinghua-Berkeley Shenzhen College doctoral student Kong Bin and Tsinghua University Shenzhen International Graduate School Master students Chen Yun and Liu Rui. The corresponding authors of the paper are Associate Research Fellow Mi Shengli and Professor Sun Wei. The research was supported by the national key research and development plan.
Link to the paper: https://doi.org/10.1038/s41467-020-14887-9
Product Details
Near-field electrospinning technology Multifunctional bio 3D printer

Multifunctional biological 3D printer is developed for tissue regeneration and repair. Tissue engineering scaffolds are beneficial to induce cell proliferation and differentiation, and can quickly promote defective tissue repair and regeneration. The multifunctional biological 3D printer can prepare scaffolds with a diameter of less than 1 micron, which is more conducive to cell attachment and differentiation.
| Features of Multifunctional Bio 3D Printer | |
| No. | Parameter characteristics |
| 1 | Printable materials: hydrogel, PCL, PLGA, PLA, chitosan, sodium alginate, temperature sensitive materials, photosensitive materials, etc.; |
| 2 | The minimum printing accuracy can reach 100nm; |
| 3 | Automatic calibration system for nozzle positioning; |
| 4 | Optional low temperature printing device; |
| 5 | Controllable environmental temperature and humidity; |
| 6 | Printing area: 150*150mm; |
| 7 | Multi-material and multi-process collaborative switching printing; |
| 8 | Stainless steel inner cavity, ultraviolet sterilization, medical cleanliness level. |
| 9 | Multiple nozzles can be switched at will; |